Protecting New Jersey
How Healthcare Facilities Helped Mount the Largest Vaccination Effort Since Polio.
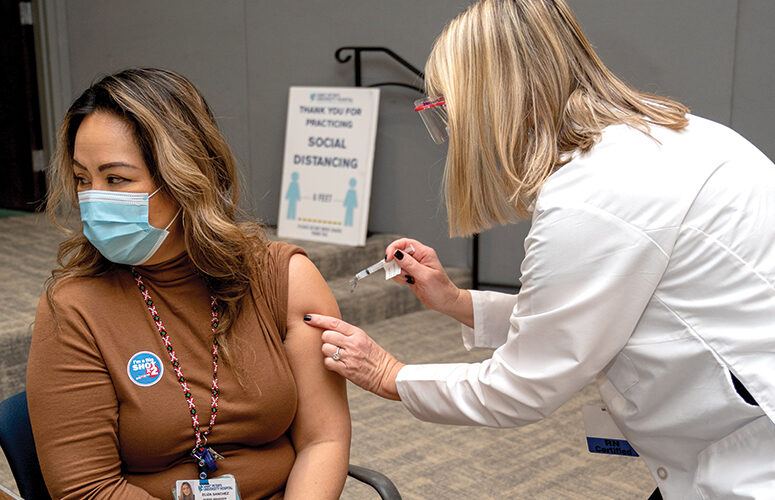
On Apr 9, 2021With a quick pinch and a jab in the arm – perhaps gratefully sporting an “I’m a Big Shot” sticker afterwards – more and more New Jerseyans are getting the COVID-19 vaccine. Behind that shot is a massive public health initiative that hasn’t been seen since 4 million Americans were inoculated against polio in 1954-1955. New Jersey’s hospitals have been a central part of that vaccination effort, giving the state a much-needed dose of hope.
New Jersey’s goal is to vaccinate 70% of the adult population within the first six months of vaccination. The state’s Department of Health designed a phased approach to vaccination, starting first with healthcare workers and nursing home residents most at risk for virus transmission, and then branching out to other populations that are most vulnerable to severe COVID-19 illness, essential workers, and ultimately the broader public as vaccine supplies increase.
As they have during the course of the pandemic, New Jersey’s hospitals and their healthcare workforce once again formed the frontlines at the state’s first vaccination sites in mid-December. Under the state’s plan, the first hospital “points of dispensing,” or PODs, were limited to healthcare workers, but as vaccine allocations began to increase, hospitals transitioned from closed PODs available only to their employees to open PODs administering the vaccine to members of their communities. Hospitals also are helping to staff and support the state’s mega-sites and community-based sites in conjunction with counties, municipalities and other local entities.
“It was a celebratory day when we began vaccinating our own employees only hours after we received the first vaccines on Dec. 17,” says Danielle Van Wert, executive director of operations integration at CentraState Healthcare System in Freehold. “We have administered tens of thousands of doses, including to eligible teachers and first responders.”
Meanwhile, New Jersey nursing homes worked in partnership with Walgreens and CVS under a separate federal program to vaccinate their residents and staff. All told, New Jersey’s long-term-care facilities provided more than 2,400 vaccination clinics from December through February to administer the vaccine to residents and staff.
Mounting a public health initiative of this magnitude – especially in healthcare sites already caring for a surge of COVID-19 patients – presented an array of challenges. The greatest? Vaccine supplies that couldn’t keep pace with the public’s demand. Allocations of the vaccine flowed from the federal government, to the states, and out to the vaccination sites. Supplies of the vaccine in the first weeks of vaccination were very limited, and while they have increased throughout late winter and early spring, there remains a long list of New Jerseyans anxiously awaiting their turn to get the vaccine.
“Probably vaccine supply was the most difficult challenge, since that is largely out of our control. We have become very well acquainted with New Jersey Department of Health (DOH) vaccine distribution officials. The DOH has a tough job and it has done an extraordinary job to get us the supply of vaccine we need,” says Lou Bezich, senior vice president of strategic alliances at Cooper University Health Care.
Cooper has supported three vaccination sites: a closed POD for its employees; an open POD in partnership with Camden County, Camden County College and Jefferson Health NJ; and a neighborhood-based vaccine and education center in the Cramer Hill section of Camden to serve a community that has been hit hard by the pandemic and that may be skeptical about receiving the vaccine.
“Our outcomes tell the story,” Bezich adds. “With our employees, we’re at 70% vaccinated and pushing for more. Our support of the Camden County site has resulted in upwards of 20,000 people vaccinated (through mid-February). And, at our new neighborhood site in Camden, we filled the available appointments for a month in just a couple of hours of opening.
“It’s been fantastic to see the response and spirit of teamwork from a number of diverse organizations to help vaccinate thousands of individuals in just a few weeks,” Bezich said.
Hospitals and health systems also faced logistical challenges, including creating an organizational structure, readying facilities, building a technical infrastructure, securing the supply chain and scheduling staff amid an ongoing public health emergency.
At Cooper, an Incident Management Team or “IMT” helped provide organizational structure to the vaccination effort. The IMT is a blend of leaders, clinicians and technicians from across the health system that reports to a medical/administrative dyad consisting of Cooper’s chief medical officer and a senior vice president, who report up to the system’s co-CEOs.
“From the beginning of the pandemic, this structure created an operating rhythm to quickly address challenges and ensure continuous reporting that facilitated sound, yet rapid decision making that was needed to keep pace with issues arising throughout the pandemic,” Bezich says.
“Like all vaccination sites throughout the state, we faced a myriad of logistical challenges in getting the vaccine in arms,” says CentraState’s VanWert. “This is new territory for all of us, and we needed to develop plans and processes very quickly – from determining the appropriate spaces in our facility to provide the vaccines, to getting adequate and appropriate staff, to determining processes for storing the vaccine. Our biggest challenge has been creating a system for taking appointment requests and handling the sheer volume of people who want vaccines, which has been complicated by the fact that we don’t have much advance information on how many vaccines we will receive or when.”
CentraState also realized that its internal call center was not going to be able to handle the volume of vaccine requests, so it quickly built a web microsite to take requests via a brief application, as well as a system to return calls and set appointments.
“Collaboration and connection to community members is essential for a successful vaccination effort,” says James A Kilmer Jr., vice president and chief administrative officer of AtlantiCare Regional Medical Center Atlantic City Campus, and incident commander of AtlantiCare’s COVID-19 Emergency Management Response Team. AtlantiCare has partnered with the state, Atlantic County and the New Jersey National Guard to support the mega-site at the Atlantic City Convention Center.
“Having strong, trusting relationships with our staff and providers, healthcare colleagues across the state, community partners, schools, state agencies, regulators and other individuals and organizations was key to addressing challenges,” Kilmer says. “Working as a team enhanced the vaccination process as we cared for all patients and each other. Individuals took on new or additional roles to support colleagues. For example, many of our non-clinical leaders and staff assisted with our staff vaccinations on their own time, including on nights and weekends. We engaged nursing and medical students in providing education and vaccinations.”
And perhaps most importantly, “We listened to learn about individuals’ concerns and questions. Rather than telling people they needed to be vaccinated, we focused on explaining how the vaccines and the FDA approval process works,” Kilmer explains.
Vaccinating New Jersey has demanded great investment in resources for the state’s healthcare vaccination sites, but has delivered a tremendous return.
“Those who do get vaccines are extremely grateful, which makes this work so rewarding,” Van Wert says. “We know we are doing our part to make our community healthier.”
Kilmer adds, “We have literally weathered every storm to get vaccines to our community during what has been the most challenging and rewarding time in most of our healthcare careers.”
To access more business news, visit NJB News Now.
Related Articles:





