New Hospital Technologies Deliver Quality & Efficient Care
Discover how the state’s healthcare institutions are implementing state-of-the-art tools to treat patients.
By Lisa Goulian Girard, Contributing Writer On Jun 13, 2016As life expectancy continues to rise in the United States – the average citizen now lives late into his or her 70s, compared to age 69 half a century ago – there’s a growing need to treat our aging population with the latest medical technology. New Jersey’s hospitals have taken on the challenge, investing in new machines that make it easier to draw blood, do gynecological surgeries with pinpoint accuracy, see the heart with 3D clarity, and treat some cancers without invasive surgery or radiation.
At the same time, there’s a new emphasis on personalized patient care and improving the hospital experience while limiting downtime. According to documents released by the Healthcare Executive Forum (HEF) at a March conference in Chicago, since 2010, healthcare has gone from being physician focused to patient focused, with patients receiving team care rather than isolated treatment as well as more access to round-the-clock services. Patient care technology is evolving similarly.
“New technology is patient centered,” says Dr. Alison Grann, chairwoman, radiation oncology, at Saint Barnabas Medical Center in Livingston. “For each patient, we have a multidisciplinary team to come up with best treatment plan based on their individual situation, which has been made possible because the science has evolved so dramatically in the last decade.”
In the past, the standard for determining whether a breast cancer patient needed chemotherapy used to be the size of the tumor: Those with a tumor over one centimeter were generally given chemotherapy, while those with a tumor under one centimeter received medication. “Thanks to new tests, we know that a tumor that measures .8 centimeter may be aggressive and require chemotherapy,” Grann says. “Similarly, we used to think all lung cancers were the same, but because of important discoveries in the last 10 years, some lung cancer patients don’t get chemotherapy, but medication.”
In January, Saint Barnabas became one of a handful of US hospitals offering M6, the latest in CyberKnife robotic radiosurgery technology. CyberKnife, which has been around since 2001, is a safe, noninvasive alternative to surgery, which delivers radiation with pinpoint accuracy to the tumor site while sparing healthy tissue surrounding the tumor. In the last 15 years, the technology has evolved and become much more precise by tracking the tumor with real-time imaging and reducing the treatment time. For the patient, it means there’s no pain, no cutting or scalpels, less toxicity, zero or minimal side effects, and reduced treatment time from one to five visits compared to 30 to 40 with conventional radiation therapy.
CyberKnife M6 technology is designed to treat both cancerous and non-cancerous tumors anywhere in the body, including the lung, prostate, brain, spine, liver, pancreas and kidney. In addition, CyberKnife is indicated for the treatment of trigeminal neuralgia and arteriovenous malformation (AVM). For many patients who do not wish to have surgery or cannot because of other health reasons, CyberKnife can be as effective as surgery. Additionally, if a patient has breast cancer or melanoma and it spreads in the form of a single tumor to the spine, that tumor can often be treated with CyberKnife as well.
Since getting the M6 machine in January, Saint Barnabas has been seeing at least 20 new consults each month. “I think the science is evolving now, which means patients get a different set of treatments than they did five years ago,” Grann says. “CyberKnife is part of the National Comprehensive Cancer Network’s (NCCN) recommendation for treatment. It’s no longer investigational, where the patient is enrolled in a clinical trial, but is there as an option along with surgery and traditional radiation.”
Life-extending cancer care has given rise to the discipline of Cardio Oncology, which is the treatment of heart conditions associated with cancer and the therapies used to treat cancer. “In the past, many patients diagnosed with cancer didn’t live long enough to develop cardio problems,” says Marcia Schaefer-Noto, MSN, RN-BC, director of cardiac services at CentraState Healthcare System, a nonprofit community health organization whose medical center is located in Freehold. “Now that many patients are surviving cancer, we need to protect their hearts from the potential effects of chemotherapeutics.”
To this end, CentraState is excited about improvements in technology for the echocardiogram, one of the most widely used diagnostic tests for patients with heart problems that shows the size and shape of the heart, pumping capacity and whether there’s tissue damage. The hospital recently unveiled the EPIC 7 ultrasound system, a 3D echocardiography machine brought to market by Royal Philips in 2013 that improves the process of evaluating the four chambers of the heart, particularly the size and function of the left ventricle.
In the last five years, echosonography technology has evolved from 2D to 3D, and the advantages of the latter are many, according to Schaefer-Noto. “3D echocardiography eliminates the need to do some of the manual measurements, which makes it more sensitive and accurate,” she says. “And when it comes to serial imaging – doing a baseline test and then repeating the test after three months or six months – it takes away the human error of measurement and allows you to recreate the same study.”
3D echocardiography is especially useful with breast cancer, gastric cancer, leukemia and lymphoma, where therapeutics can be harmful to the heart. It helps measure how the heart is doing before, during and after therapies, and 3D shows how the heart pumps, detecting very small changes in its structure. 3D echo is also used for clinical decision making or prognosis of patients with valvular problems, as it allows doctors to see how well valves are able to push blood out and detects changes in the heart that can lead to heart failure. In addition, the technology can be used for pre-surgical workups for patients who are about to undergo bypass or other surgeries.
CentraState is in the process of training staff to use the EPIC system and rolling it out to physicians so “we can offer the best testing out there on the market today,” Schaefer-Noto says. “The whole area of cancer therapeutics is evolving, and we want to provide our patients with the most advanced technologies for optimizing not only their cancer treatment, but their overall health.”
Monmouth Medical Center in Long Branch has also invested in 3D technology – this time in the form of robotic-assisted gynecological surgeries. Long known for excellence in the area of laparoscopic hysterectomy (the surgical removal of a woman’s uterus), the hospital spent more than $1 million on a da Vinci robot in 2006. Over the last 10 years, the team has added to the basic platform, leading to more precise and less invasive gynecological surgeries.
“There has long been debate over the safety of laparoscopic surgery compared to other surgeries,” says Dr. Robert A. Graebe, chairman of obstetrics and gynecology at Monmouth Medical Center, an RWJBarnabas Health facility, as well as the director of residency and division head of reproduction and fertility. “Newer literature is leaning toward the fact that with advances in the technology and the accumulation of experience with robotics, it’s starting to overwhelm traditional surgery.”
Laparoscopic hysterectomy is done through small incisions using a thin, lighted scope with a camera on the end. With the robotic machine, the surgeon sits at a computer station and controls the surgical instruments very precisely, which gives true depth perception and makes it easier to move into tiny spaces. More recently, the technology has evolved to include improved vessel sealing, ultrasound devices as well as devices that utilize tissue fluorescence.
“Every surgeon has a little tremor to his or her hand; the robot removes it. The physician sits at a console, so fatigue is reduced,” Graebe says. “This is all helpful to the surgeon, which means it’s good for the patient.” In addition to a marked decrease in surgical time, size of surgical wounds and blood loss, use of this technology shaves days off hospitalization and weeks off recovery.
And while it generally takes about four years to learn to perform traditional laparoscopic surgery, a doctor can become proficient on the robot in about six months, according to Graebe. “The new generation – those surgeons who don’t know a time before cell phones, computers or robots – moves into technology quickly and in a robust way, and they do very well with it,” he says. “All our residents graduate with proficiency in robotics.”
The gynecological team at Monmouth, led by Drs. Hackett, Kolomeyevskaya, Michalewski, Henderson and Eswar, has performed more than 1,500 surgeries in the past 10 years – not only hysterectomies, but myomectomies and repairing of tubes and ovaries. The hospital has since added a second da Vinci robot, and the technology has been used for an additional 1,500 surgeries in other hospital departments.
“The future is in the advancement of technology for patient safety, and we are constantly reading about and developing technology that we feel is safe, effective and efficient for patient use,” Graebe adds. “It’s not about technology for technology’s sake, but technology proven to be efficacious for the patient. Robotics have the most potential for advances.”
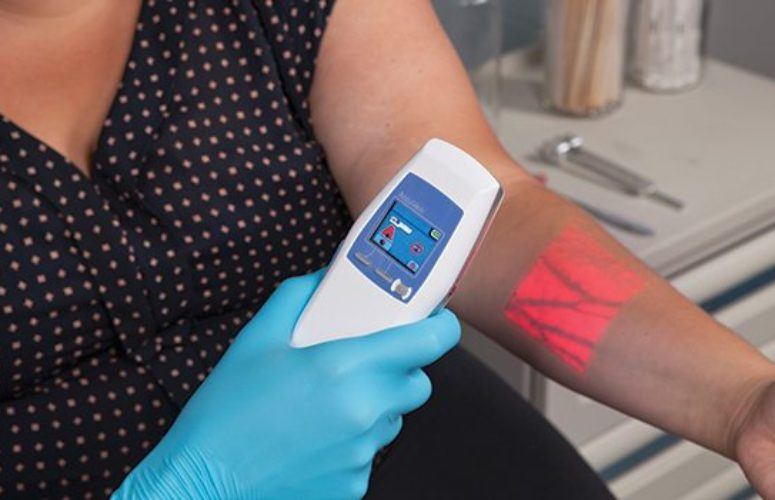
Also in the area of patient care, The Valley Hospital in Ridgewood is trying to ease the process of drawing blood or inserting an IV, particularly for those with hard-to-reach veins who have experienced multiple needle sticks before therapy is initiated. The hospital has invested in the AccuVein illumination device, a small hands-free unit that, when held above the skin, lights up veins like a roadmap. As hemoglobin in the blood absorbs the infrared light, veins appear noticeably different than the surrounding tissue, aiding in vein location to collect a blood sample or administer IV medications.
Different organizations, including the Infusion Nurse’s Society, are recommending it as a best practice for finding veins, not only in high-risk patients, but as a general guideline. “A lot of people have anxiety and fear about getting needles, and this can add comfort to that process,” says David Rivera, director of cardiac services at Valley Hospital’s Heart & Vascular Institute. “Vein illumination is considered a modality for higher risk patients. It allows the patient comfort that finding a vein is going to be successful in one stick, and one try is always best for patient satisfaction and comfort.”
Valley started using AccuVein technology in 2014 in Pediatrics (“small children, small veins”), and initial success deemed the device appropriate for other hospital populations. The major rollout of about 20 devices began in September, with each device carrying a suggested retail price of $5,500.
“With the aging population, and complex co-morbities, it makes those individuals more difficult for IV therapy and blood drawing,” Rivera says, who added that AccuVein is being used on a growing percentage of the hospital’s patients, including older people with torturous (crooked) veins, people who are morbidly obese, people with darker skin tones, and those affected by dehydration, certain medications or drug abuse.
Vein illumination technology, which is also being offered by competing brands, has not only been adopted by The Valley Hospital, but by other hospitals in Northern New Jersey and Metro New York. The technology continues to be improved, as the medical community tries to advance the IV catheter to make insertion easier, Rivera says. AccuVein also addresses the trend toward portable, less invasive devices that provide the best data to make decisions. “People can clip cases to their iPhone and get a recording of their heart rhythm to send to their cardiologist,” Rivera adds. “Patients are getting feedback on their own health and body and acting on it.”
This idea of tracking patient health through technology is being advanced in a big way by Hackensack University Medical Center (HackensackUMC). The hospital has made strides in the area of digitalization of electronic health records, as putting all records and treatments online can make healthcare more proficient – and more personal.
“We see it as a whole care continuum, following the patient his or her whole life,” says Dr. Shafiq Rab, CIO for HackensackUMC, whose work in this area earned him the 2015 Innovator of the Year Award from the College of Healthcare Information Management Executives. “If we keep on top of things and can prevent bad things from happening, people will be less ill and require less surgery – which keeps costs down.”
HackensackUMC is one of the first US hospitals working with Apple, Google and Microsoft to link patient-generated data from mobile apps and personal fitness devices like the Apple iWatch to a centralized system that gives doctors a more complete picture of a patient’s health and care. The hospital has been using the Infor Cloverleaf Integration Suite to develop and implement open, vendor-neutral or Fast Healthcare Interoperability Resources (FHIR) standards.
“How do we provide a person access whenever they want, wherever they want, and make it easy and secure?” Rab poses. “It starts with the digitalization of electronic health records. And this involves getting past the firewalls built into certain applications and making things universal.”
The addition of information and service extends from that basic premise. For example, if a patient is supposed to walk five miles a day, his Apple iWatch will send his distance traveled to his iPhone, which will integrate it into a central database. The same can be said for a digital scale, which can generate useful information about a patient’s weight loss or gain directly to his or her physician.
HackensackUMC also offers an app where patients can now make an appointment at their leisure. They can upload their photo ID and insurance card to a portal called My Chart, which checks the group number, benefits and health records. There is technology to direct your car to the hospital, check you in at the gate and provide a video of the hospital so you don’t get lost. In addition, new moms can see their babies from their hospital bed via video.
“We also provide free Wi-Fi for loved ones in the waiting area and, if admitted to the hospital, the patient gets a tablet where he or she can watch Netflix, order food, etc.,” Rab says. “What it all means is we are using technology to enhance the experience of the patient. We want to earn their respect because we are not only taking care of them as a patient, but as a human being.”
The trend toward making things easier for patients can also be seen in bedside ultrasound, which is being used at Kennedy University Hospitals on a daily basis in its Intensive Care Units. While initially used simply to increase the safety of vascular access procedures, technological improvements to the equipment and advanced training for physicians have allowed bedside ultrasounds to become integral in a wide array of diagnostic and therapeutic procedures at Kennedy. These include evaluating overall heart function, valve pathology, and aiding with the detection of fluid surrounding the heart.
“Bedside ultrasound of the lung can now help us differentiate heart failure from pneumonia, as well as assist in making a rapid assessment of a collapsed lung – all without radiation exposure to a patient from a chest x-ray,” says Kelly A. Schiers, DO, Kennedy Health Alliance ICU medical director. “By placing the ultrasound probe on someone’s abdomen, we can find infected fluid or bleeding. A quick exam of the lower extremities can aid in the discovery of blood clots that could become life-threatening, and ultrasound of the eye can even uncover elevated pressures in the brain.”
While various forms of ultrasound have been around since the 1950s, bedside ultrasound has become an integral part of ICU care in the last few years, made possible by smaller machines, decreased cost and vastly improved image quality.
Kennedy has ICU-based ultrasound equipment at its Cherry Hill and Straford locations, and there are three ultrasound machines in the ICUs at the Washington Township facility, including a state-of-the-art Sonosite X-Porte that provides the most advanced quality images as well as technology that allows these images to be directly loaded into a patient’s electronic medical record.
Additionally, the Kennedy Health Alliance, a network of primary and specialty care physician practices located throughout southern New Jersey, is also in the process of purchasing a tablet-sized ultrasound that can be taken to a patient’s bedside anywhere in the hospital, allowing the ICU team to perform an evaluation on the general medical floor.
“Bedside ultrasound allows us to bring equipment to the patient, as opposed to bringing the patient to the equipment,” Schiers says. “ICU patients are the sickest in the hospital, and whenever we can limit moving them from under the watchful eyes of the ICU physicians and nurses, patient care is improved.”
In addition, bedside ultrasound can increase the speed of achieving a diagnosis or performing a procedure. “For years now, we know from various studies that direct visualization provided by ultrasound imagining increases success rates and limits potential complications during routine ICU procedures,” she adds. “And finally, but certainly no less important, bedside ultrasound can replace x-ray and CT imaging in certain circumstances, allowing us to limit radiation exposure for patients.”
Related Articles: